Intradiscal Regernerative Medicine
Live Life Pain Free
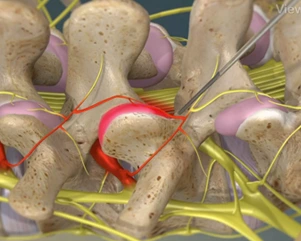
Percutaneous discectomy is a minimally invasive procedure used to treat herniated disks. The goal of the procedure is to relieve pain by removing pressure on the nerve root. During percutaneous discectomy, a small incision is made in the back, and a thin tube called a cannula is inserted into the space between the vertebrae. Using fluoroscopic guidance, the surgeon then inserts a needle-like device through the cannula and into the herniated disk. The disk is then fragmentized with heat or laser energy and removed through the cannula. Percutaneous discectomy is generally safe and effective, and most people experience significant relief from their symptoms after the procedure. Recovery times vary depending on the individual, but most people can return to their normal activities within a few weeks. However, it is important to note that percutaneous discectomy is not a cure for herniated disks, and there is a risk of recurrence. If you are experiencing pain from a herniated disk, talk to your doctor to see if percutaneous discectomy might be right for you.
Identify and Treat your back pain with disc decompression
A herniated disc can negatively affect your ability to perform everyday activities. If your discomfort isn’t improving with conservative treatments—bed rest, pain medication, stretching or cold and/or heat therapy—disc decompression may be your best option. It has a high success rate and low complication rate.
What are some symptoms and causes that may require disc decompression?
Leg Pain Symptoms
- Usually occurs in only one leg
- May starts suddenly or gradually
- May be constant or may come and go
- May get worse when sneezing, coughing or straining during bowel movements
- May be aggravated by sitting, prolonged standing and bending/ twisting
Nerve-Related Symptoms
- Tingling (“pins-and-needles” sensation) or numbness in one leg
- Weakness in one or both legs
- Pain in the front of the thigh
What are the benefits of Percutaneous Discectomy?
- Significant pain relief
- Reduced use of pain medication
- Return to previous levels of activity
- Less scarring
- Quick recovery
- Low complication and morbidity rates
What are the results compared to surgery?
- Decreased complication rate compared to open surgical discectomy
- Lower re-herniation rate compared to open lumbar discectomy
Educational Videos
Click On The Links Below To Watch Educational Videos
Book An Appointment
Fields Marked With An ” *” Are Required